Artificial Intelligence (AI) in Dermatology Education: Comparative Study with Medical Students

Summary
Over a 3 month period we conducted an online diagnostic dermatology survey with medical students in their 4th year that had undergone a two week dermatology program. We had Group A that consisted of 10 medical students that only had access to patient history and two images of the skin disease. They were compared to Group B that consisted of 10 medical students that had access to the same information, but also Autoderm version 2.2 top 5 AI answers to assist them. They were judged on diagnostic accuracy, treatment management, if they should refer the patient and how long it took them to answer the cases.
Introduction
Artificial Intelligence (AI) is revolutionizing education and clinical medicine, opening doors to new possibilities. AI in dermatology education enhances how we screen for health conditions, diagnose illnesses, and medical education by offering customized and efficient approaches. This cutting-edge technology is especially beneficial for medical students, as it provides them access to advanced diagnostic tools and personalized learning experiences, helping them understand and diagnose skin conditions better.
AI-Driven Enhanced Diagnostic Accuracy and Dermatology Learning
AI powered by convolutional neural networks (CNN) is emerging as a major turning point in dermatology. These advanced neural networks are specially designed for image processing, making them incredibly effective at analyzing and diagnosing skin conditions with impressive accuracy.1 Because of these qualities, medical students can compare the AI generated diagnoses with their own and improve their diagnostic accuracy. Most AI algorithms are trained using a vast collection of data, including pictures and details of different skin conditions. This database can be utilized for learning purposes for the medical community. AI can simulate cases based on this data, and medical students can practice diagnosing and managing different conditions, gaining experience and confidence.
Personalized Learning in Dermatology Education with AI
The potential of AI in education is truly exciting, especially when it comes to tailoring learning materials to fit each student's unique needs. By adapting to individual preferences—like readability, language level, or even the speed of a speaker—AI can create a personalized learning experience that is more engaging and accessible for everyone. This includes those with disabilities as well.2 It can also be used to generate tailored recommendations, such as specific videos, articles and cases based on individual performance, so the students can focus more on the areas they need improving the most.
Real-Time Feedback and AI-Powered Assessment in Medical Education
Another important feature of AI is the ability to provide instant, interactive feedback, helping students reinforce their knowledge effectively and in real-time.3 This hands-on, responsive learning style not only makes studying more engaging but also deepens understanding in a way that's both meaningful and memorable. Wang et al. Provide evidence as to how AI technology is transforming the way we track student performance, offering a continuous and integrated approach throughout the teaching and learning process.4 Furthermore, with predictive analytics, educators can identify students who may be at risk of struggling or dropping out, allowing for early intervention and support.5
AI Access to the Latest Dermatology Research and Guidelines
AI offers medical students unparalleled access to the latest research and guidelines in dermatology, curating and summarizing up-to-date information. By delivering customized content tailored to their interests, AI keeps students informed and engaged with the most current developments in the field.
Improving Clinical Skills with AI in Dermatology Training
AI-powered virtual assistants can guide students through clinical procedures, offering step-by-step instructions and emphasizing critical points. Many studies have been conducted on simulation-based learning, where medical students and practitioners can use AI generated virtual environments to practice and assess clinical skills such as surgery.6 Similarly, AI can simulate rare dermatological conditions, giving students the chance to learn about and identify less common diseases they might not frequently encounter in clinical practice.
AI-Enabled Collaboration and Global Knowledge Sharing in Dermatology
AI opens the doors for collaborative learning on a global scale by connecting students with peers and experts from around the world.6 This technology enables students to share cases, discuss diagnoses, and learn from a diverse community. With interactive case discussions, AI not only organizes and moderates these sessions but also ensures that they are focused and cover essential learning points, making the learning experience more engaging and productive.
AI-Enhanced Clinical Decision Support in Dermatology Training
AI can be a helpful guide in clinical decision-making, offering suggestions for possible diagnoses and treatment options based on the information provided. This feature not only supports students but also helps them learn and understand how medical decisions are made in practice. According to a study by Cheng CT, et al., AI-assisted images in medical education and diagnostics have shown to give more accurate clinical assessment results compared to traditional methods.7
Furthermore, AI can help students learn to integrate patient data from Electronic Health Records (EHR) into their diagnostic and treatment planning, making these processes smoother and more informed, while also using raw data from EHRs to develop prognostic models for better patient care.8
Optimizing Time Management and Efficiency with AI in Medical Training
AI significantly enhances time management and efficiency in medical education. By taking over automated administrative tasks like scheduling, documentation, and data entry, AI frees up students' time, allowing them to concentrate more on learning and patient care. Additionally, AI can streamline study plans by pinpointing high-yield topics and tailoring study schedules to align with exam dates and curriculum needs, ensuring a more focused and productive learning experience.
Final Thoughts on AI's Impact in Dermatology Education
In conclusion, the integration of AI in dermatology education offers a transformative approach, enhancing diagnostic accuracy, personalized learning, and clinical skills. AI's ability to provide real-time feedback, access to the latest research, and streamlined study plans empowers medical students to excel. As AI continues to evolve, its role in medical education will likely expand, providing even greater support and opportunities for future healthcare professionals.
Study Methodology
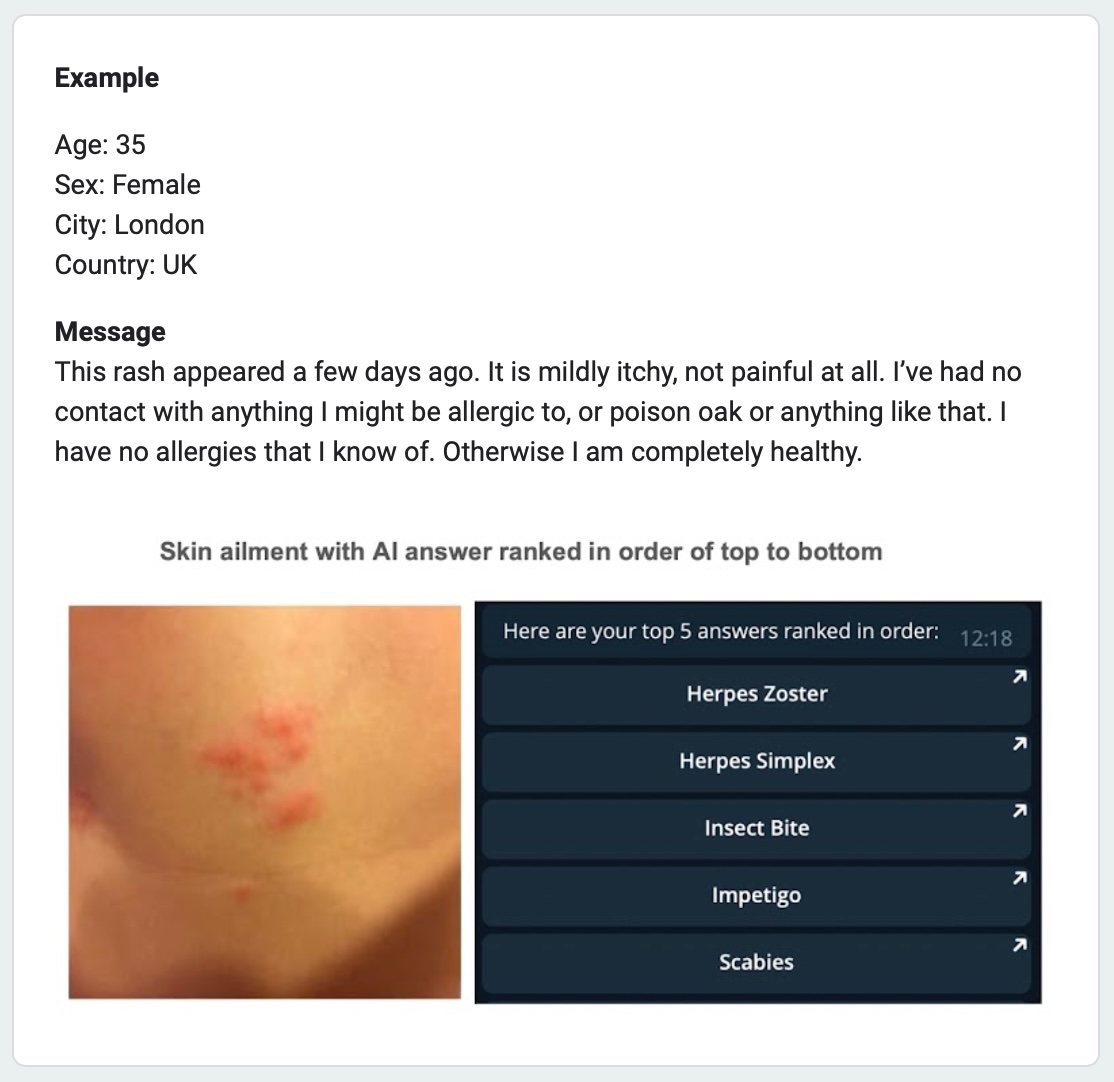
An online questionnaire (Google Survey) containing questions on 20 different dermatology cases was compiled with an overview image and a close-up image of skin lesions sent to the First Derm online platform, including a brief clinical description provided by the patients (Figure 1). The following areas of inquiry were used to collect data.
- Three differential diagnoses in the order of probability
- Recommendations on management
- Opinion on dermatologist/GP referral/ self treatment
- Time spent on each case
A second questionnaire was made using the same questions on the same cases, with the addition of 5 possible AI generated answers ranked in order using Autoderm version 2.2. (Figure 2).
Two groups of medical students were instructed to review the details provided, and answer the questions. Ten medical students received a questionnaire with 2 images and describing text of the patient's concern (Group A). A second group of 10 medical students received the same information and an AI assistance answer on the case (Group B). Each student was advised to fill out the online questionnaire based on their knowledge, while the Group B students had the opportunity to look at the AI generated answers and take the information into consideration when forming their own diagnoses.
At the end of the survey, information on the level of difficulty was obtained from both groups, while additional information on helpfulness of AI assistance in diagnosing the conditions, and opinion on using AI assistance were collected from the Group B students.
Correct diagnoses of the cases were obtained from board certified dermatologists via the First Derm online platform, to help determine the diagnostic accuracy of study and control groups. The data obtained from the two groups were assessed to determine the comparative accuracy of differential diagnoses, management recommendations and time spent on each case.

Results
1. Top Diagnosis Accuracy
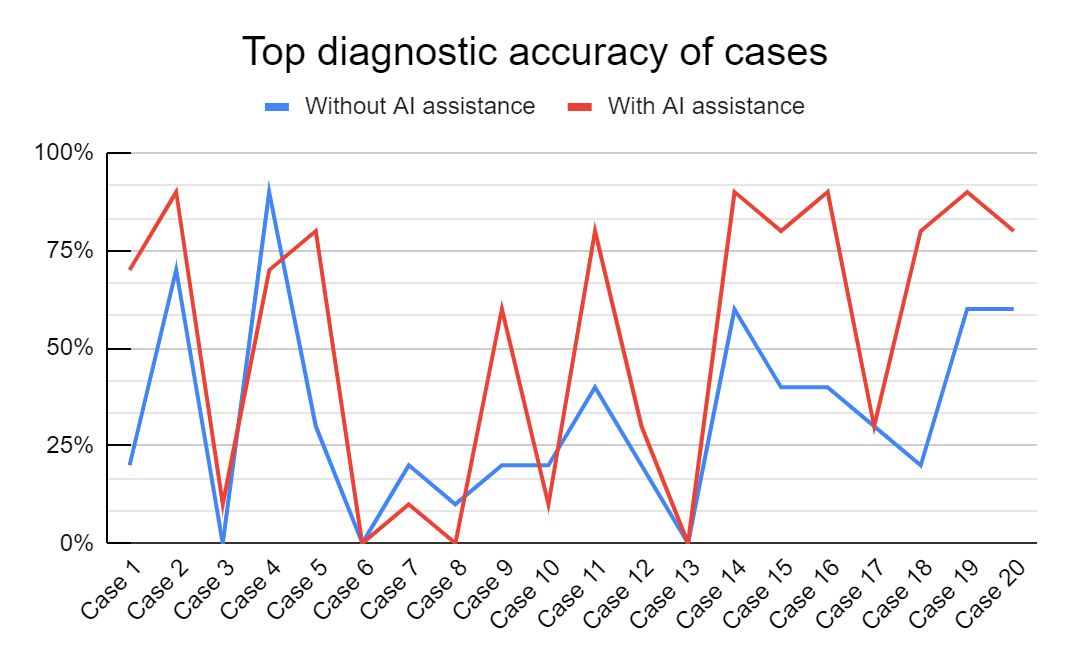
The top diagnostic accuracy of 14 out of 20 cases were increased with AI assistance. 3 out of 20 cases had similar accuracy in both groups. The variation in accuracy in individual cases with and without AI assistance is shown in the graph below. (Figure 3)
2. Accuracy of top 3 differential diagnoses
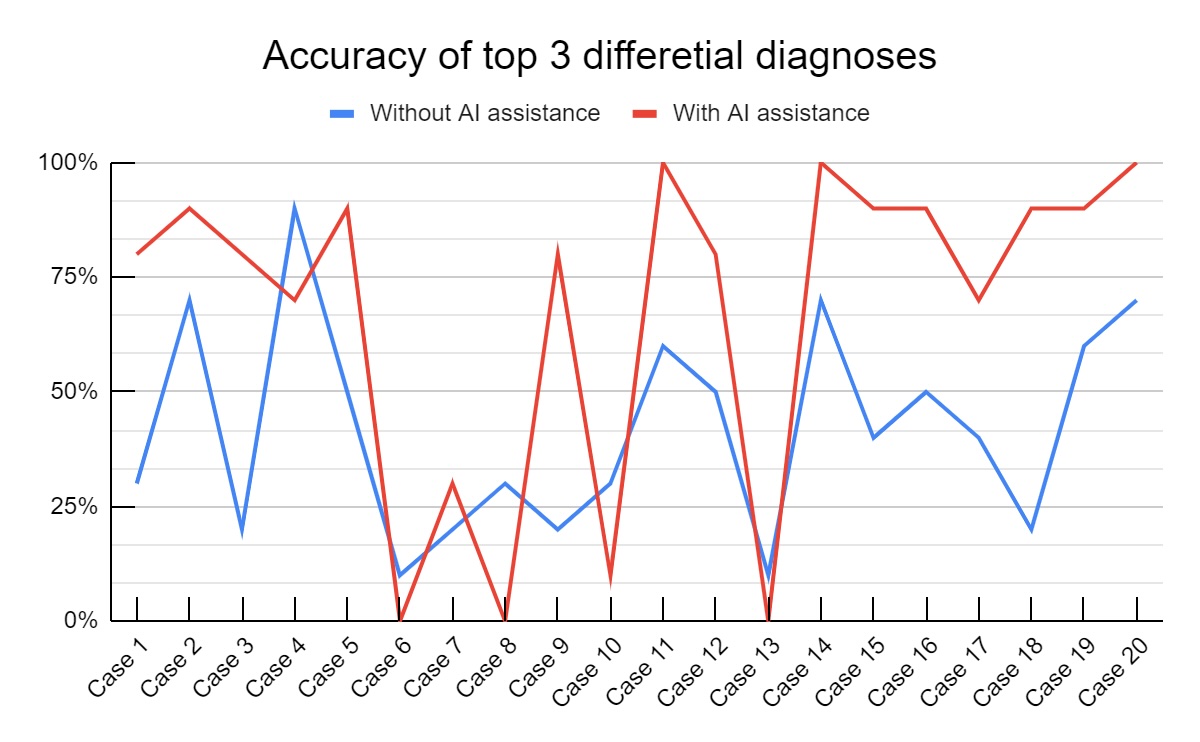
The accuracy of top 3 differential diagnoses of 15 out of 20 cases were increased with AI assistance. The variation in accuracy of top 3 differential diagnoses in individual cases with and without AI assistance is shown in the graph below. (Figure 4)
Accuracy of management recommendations
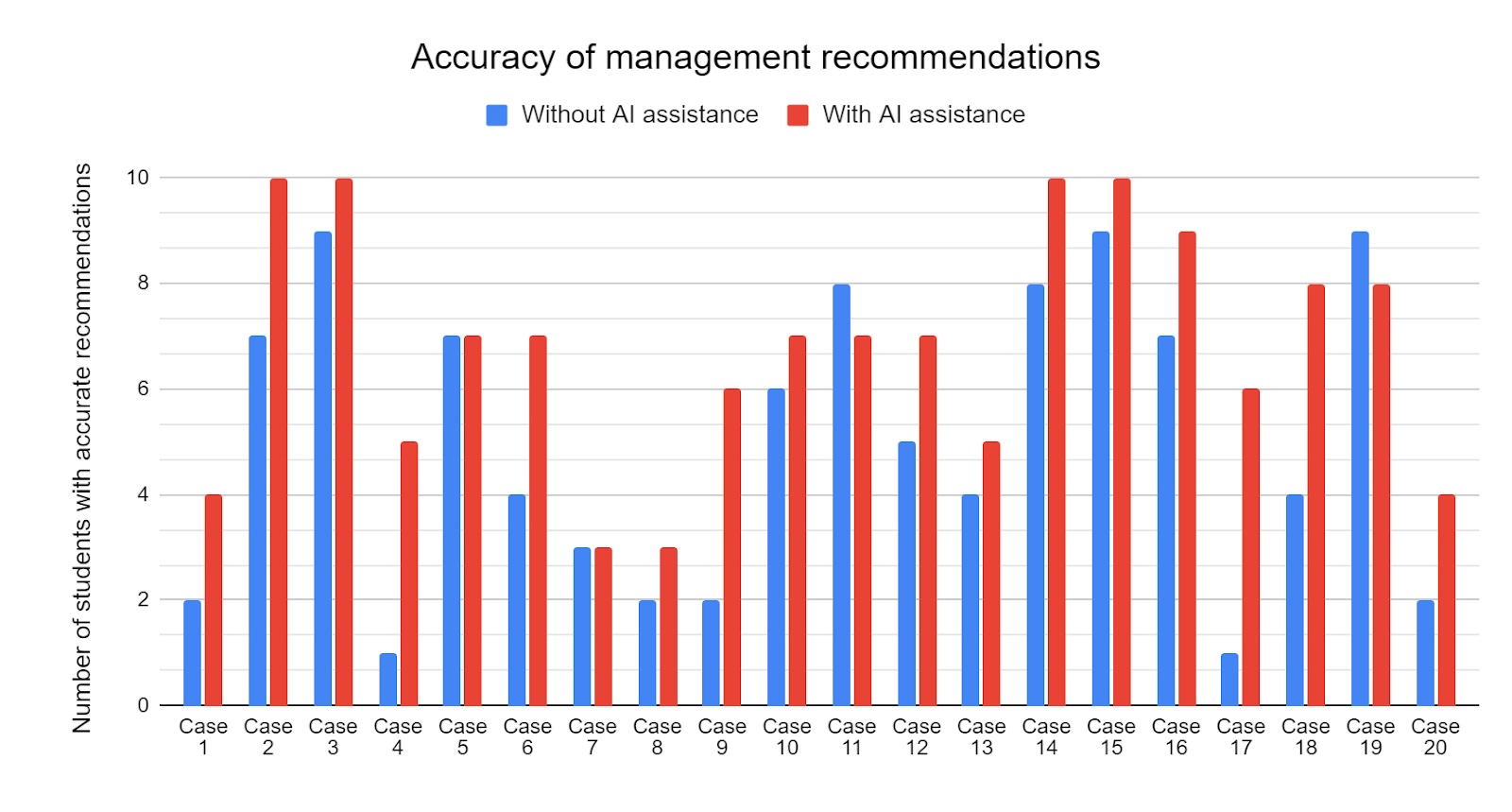
Details on management recommendations including several classes of medication (eg: antibiotics, antifungals, moisturiser, corticosteroids) were obtained and compared to the dermatologists' recommendations. In 16 out of 20 cases, the recommendations were more accurate in the study group with AI assistance, while 2 out of 20 cases showed similar accuracy in both groups. (Figure 6)
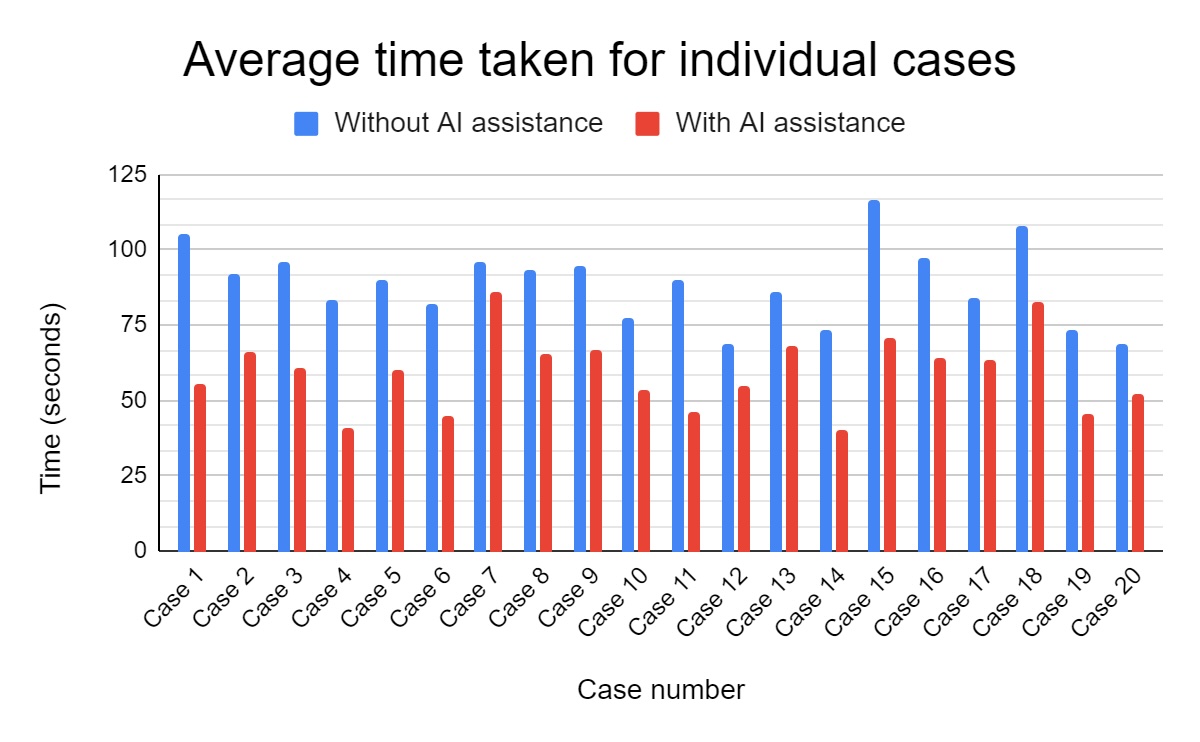
Time taken for diagnosis and recommending management options
The average time spent on each case was significantly reduced in the study group with AI assistance, compared to the control group. (Figure 7)
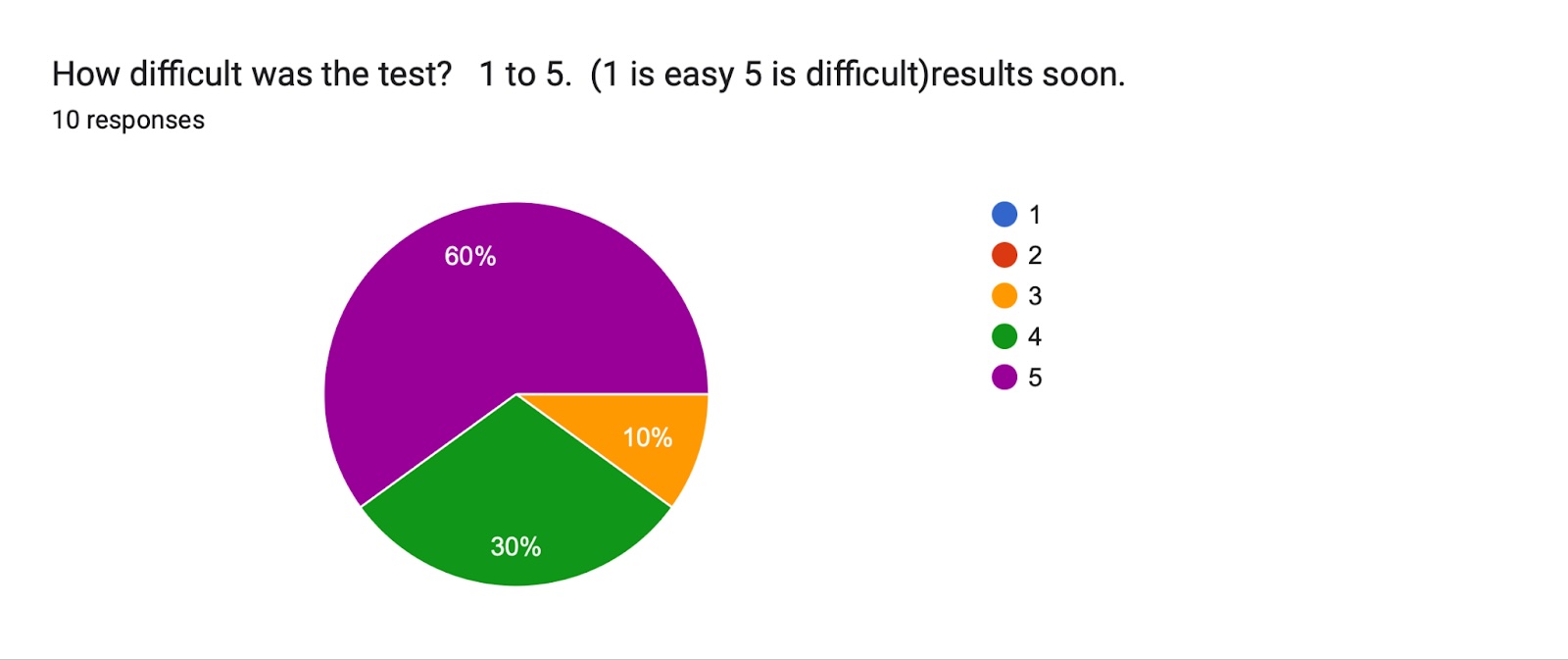
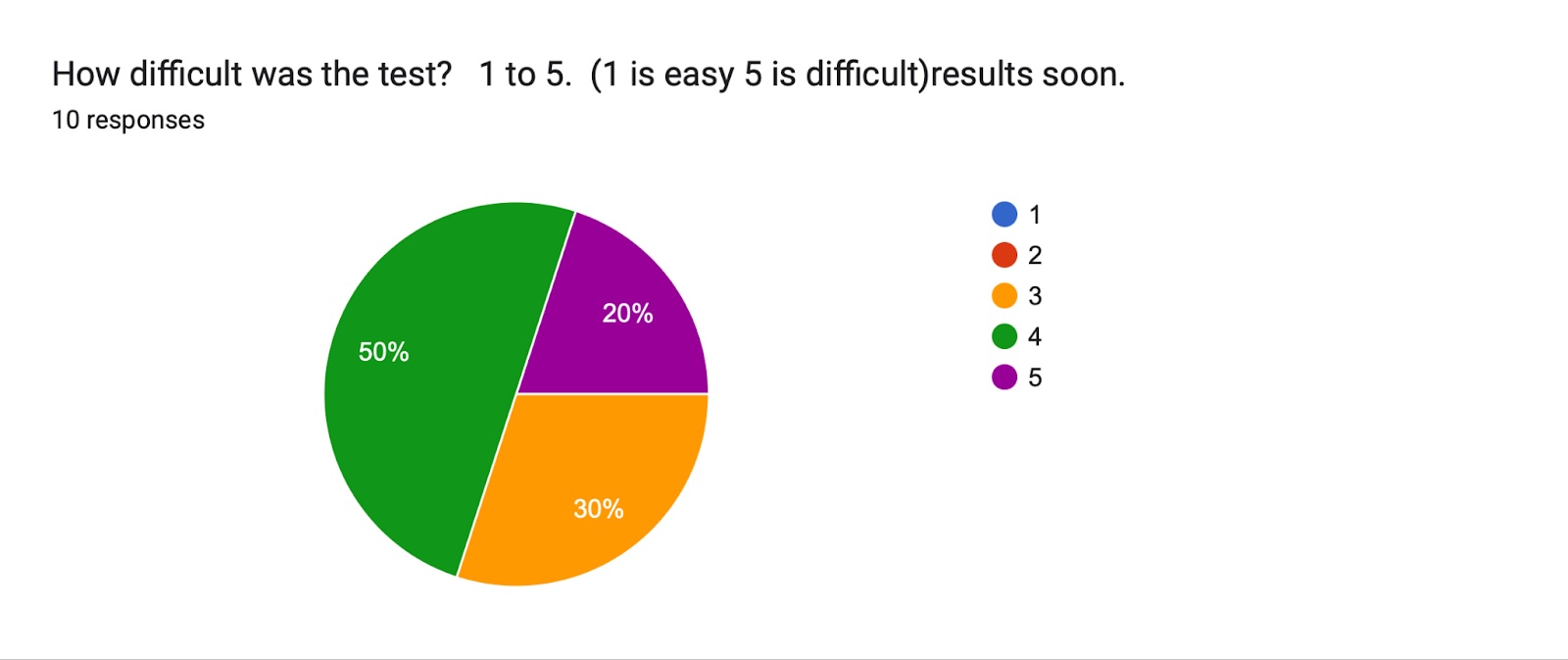
Students' feedback
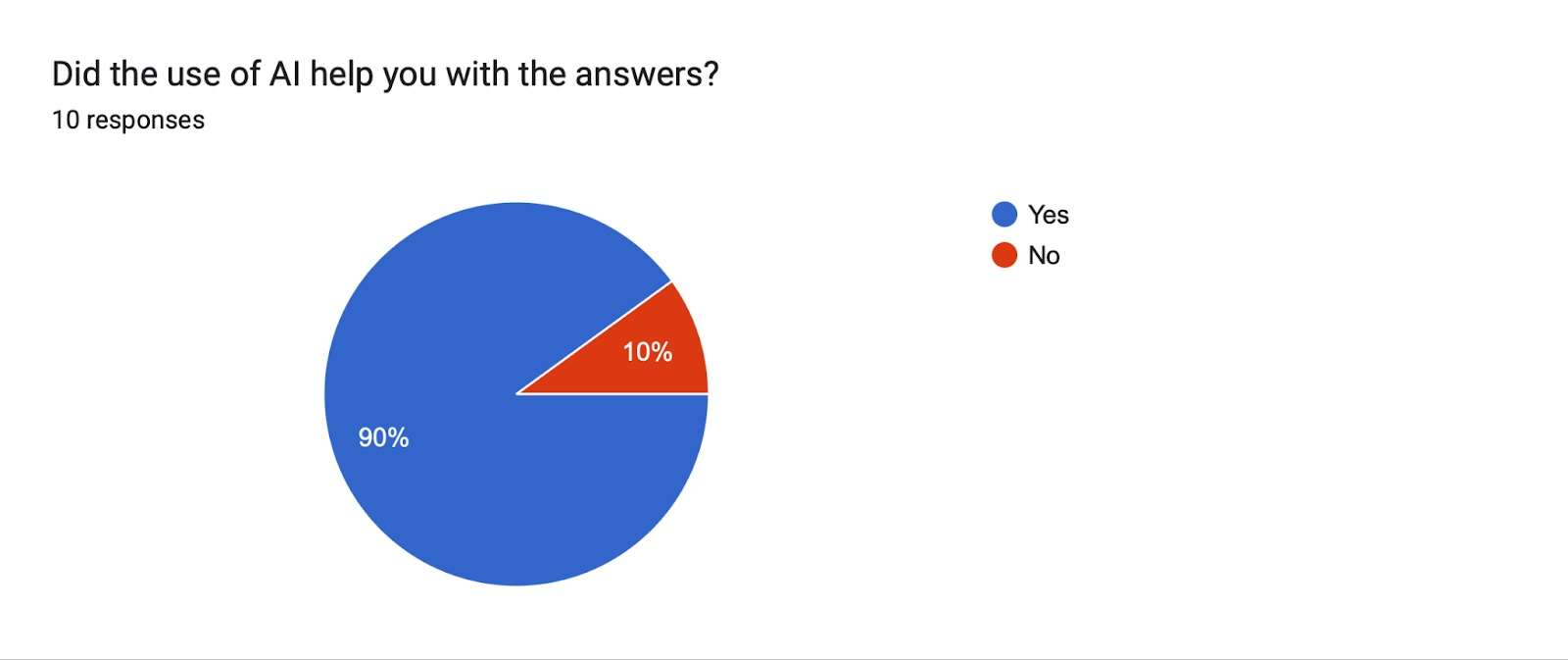
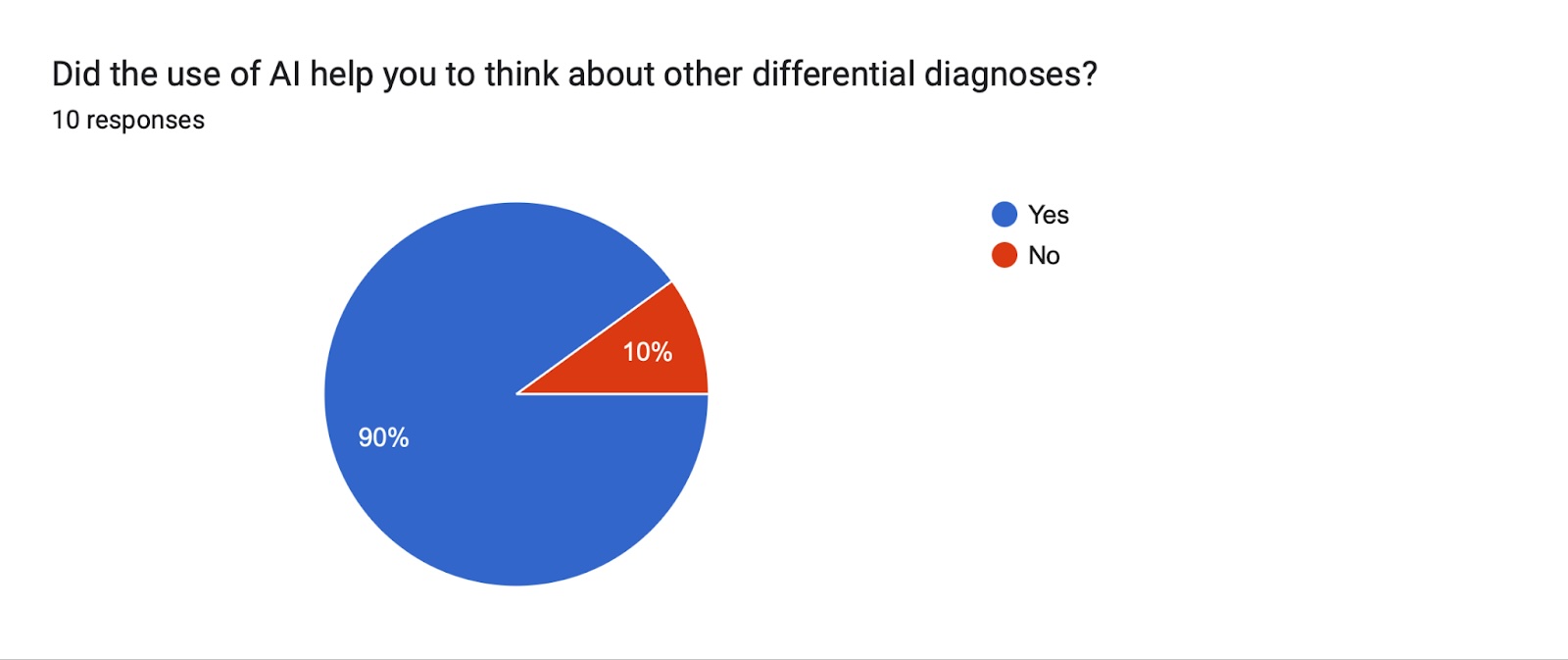
Majority of the participants in the study group who received AI assistance had positive feedback on performance and utility of AI. 4 out of 10 students claimed the use of AI alone would have been sufficient to resolve the consultation. 9 out of 10 students confirmed that they used the assistance given by the AI in completing the survey, and confirmed that the use of AI helped them to think about other differential diagnoses. 8 out of 10 students stated that they would use the AI in similar settings. The level overall of difficulty as recorded by the students was higher in the control group who did not receive any AI assistance. Overall, the study group with AI assistance completed the task with better accuracy and more efficient time management than the control group.
Discussion
This study assessed the impact of AI assistance on the diagnostic accuracy, management recommendations, and time efficiency of medical students in dermatology cases. Group A spent more time on the cases, got more diagnoses wrong, treatment wrong than Group B that had patient history and an AI assistant answer.
Key Findings
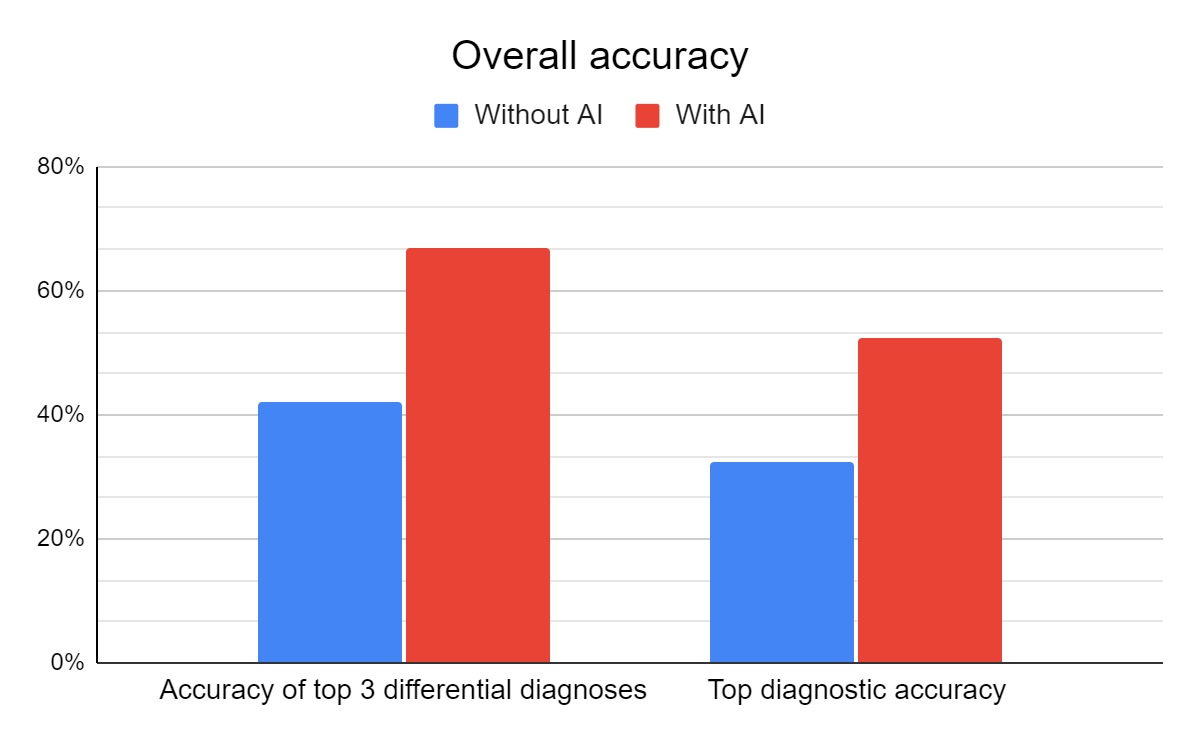
- Diagnostic Accuracy: AI assistance improved the top diagnostic accuracy in 14 out of 20 cases (75%) and improved the accuracy of the top three differential diagnoses in 15 out of 20 cases (75%).
- Management Recommendations: The AI-assisted group provided more accurate management recommendations in 16 out of 20 cases (75%), with similar accuracy in two cases.
- Time Efficiency: AI assistance significantly reduced the time spent on diagnosis and management compared to the control group (40%).
- Student Feedback: In general they thought the test was difficult, however Group B students thought it was less difficult when they had access to the AI assistant's answer. Most students found the AI to be useful when considering alternative diagnoses. Ninety percent of the medical students indicated they would use AI in a future diagnostic setting.
Conclusion
Overall, the AI-assisted group outperformed the control group in terms of diagnostic accuracy, efficiency, and decision-making confidence. This suggests that AI can be a valuable tool in enhancing medical education and clinical practice.
References
- Alex Krizhevsky, Ilya Sutskever, and Geoffrey E. Hinton. 2017. ImageNet classification with deep convolutional neural networks. Commun. ACM 60, 6 (June 2017), 84–90. https://doi.org/10.1145/3065386
- Bulathwela S, Pérez-Ortiz M, Holloway C, Cukurova M, Shawe-Taylor J. Artificial Intelligence Alone Will Not Democratise Education: On Educational Inequality, Techno-Solutionism and Inclusive Tools. Sustainability. 2024; 16(2):781. https://doi.org/10.3390/su16020781
- Sohail N, Puyana C, Zimmerman L, Tsoukas MM. AI in Dermatology: Bridging the Gap in Patient Care and Education. Clin Dermatol. Published online June 25, 2024. < href="https://doi:10.1016/j.clindermatol.2024.06.009" target="_blank">https://doi:10.1016/j.clindermatol.2024.06.009
- Wang T, Lund BD, Marengo A, Pagano A, Mannuru NR, Teel ZA, Pange J. Exploring the Potential Impact of Artificial Intelligence (AI) on International Students in Higher Education: Generative AI, Chatbots, Analytics, and International Student Success. Applied Sciences. 2023; 13(11):6716. https://doi.org/10.3390/app13116716
- Igbokwe, I.C., 2023. Application of artificial intelligence (AI) in educational management. International Journal of Scientific and Research Publications, 13(3), pp.300-307. https://www.ijsrp.org/research-paper-0323.php?rp=P13512782
- Sapci AH, Sapci HA. Artificial Intelligence Education and Tools for Medical and Health Informatics Students: Systematic Review. JMIR Med Educ. 2020;6(1):e19285. Published 2020 Jun 30. https://mededu.jmir.org/2020/1/e19285/
- Cheng CT, Chen CC, Fu CY, et al. Artificial intelligence-based education assists medical students' interpretation of hip fracture. Insights Imaging. 2020;11(1):119. Published 2020 Nov 23. https://insightsimaging.springeropen.com/articles/10.1186/s13244-020-00932-0
- Liopyris, Konstantinos, et al. "Artificial intelligence in dermatology: challenges and perspectives." Dermatology and Therapy 12.12 (2022): 2637-2651. >https://link.springer.com/article/10.1007/s13555-022-00833-8
Summary
Over a 3 month period we conducted an online diagnostic dermatology survey with medical students in their 4th year that had undergone a two week dermatology program. We had Group A that consisted of 10 medical students that only had access to patient history and two images of the skin disease. They were compared to Group B that consisted of 10 medical students that had access to the same information, but also Autoderm version 2.2 top 5 AI answers to assist them. They were judged on diagnostic accuracy, treatment management, if they should refer the patient and how long it took them to answer the cases.
Introduction
Artificial Intelligence (AI) is revolutionizing education and clinical medicine, opening doors to new possibilities. AI in dermatology education enhances how we screen for health conditions, diagnose illnesses, and medical education by offering customized and efficient approaches. This cutting-edge technology is especially beneficial for medical students, as it provides them access to advanced diagnostic tools and personalized learning experiences, helping them understand and diagnose skin conditions better.
AI-Driven Enhanced Diagnostic Accuracy and Dermatology Learning
AI powered by convolutional neural networks (CNN) is emerging as a major turning point in dermatology. These advanced neural networks are specially designed for image processing, making them incredibly effective at analyzing and diagnosing skin conditions with impressive accuracy.1 Because of these qualities, medical students can compare the AI generated diagnoses with their own and improve their diagnostic accuracy. Most AI algorithms are trained using a vast collection of data, including pictures and details of different skin conditions. This database can be utilized for learning purposes for the medical community. AI can simulate cases based on this data, and medical students can practice diagnosing and managing different conditions, gaining experience and confidence.
Personalized Learning in Dermatology Education with AI
The potential of AI in education is truly exciting, especially when it comes to tailoring learning materials to fit each student's unique needs. By adapting to individual preferences—like readability, language level, or even the speed of a speaker—AI can create a personalized learning experience that is more engaging and accessible for everyone. This includes those with disabilities as well.2 It can also be used to generate tailored recommendations, such as specific videos, articles and cases based on individual performance, so the students can focus more on the areas they need improving the most.
Real-Time Feedback and AI-Powered Assessment in Medical Education
Another important feature of AI is the ability to provide instant, interactive feedback, helping students reinforce their knowledge effectively and in real-time.3 This hands-on, responsive learning style not only makes studying more engaging but also deepens understanding in a way that's both meaningful and memorable. Wang et al. Provide evidence as to how AI technology is transforming the way we track student performance, offering a continuous and integrated approach throughout the teaching and learning process.4 Furthermore, with predictive analytics, educators can identify students who may be at risk of struggling or dropping out, allowing for early intervention and support.5
AI Access to the Latest Dermatology Research and Guidelines
AI offers medical students unparalleled access to the latest research and guidelines in dermatology, curating and summarizing up-to-date information. By delivering customized content tailored to their interests, AI keeps students informed and engaged with the most current developments in the field.
Improving Clinical Skills with AI in Dermatology Training
AI-powered virtual assistants can guide students through clinical procedures, offering step-by-step instructions and emphasizing critical points. Many studies have been conducted on simulation-based learning, where medical students and practitioners can use AI generated virtual environments to practice and assess clinical skills such as surgery.6 Similarly, AI can simulate rare dermatological conditions, giving students the chance to learn about and identify less common diseases they might not frequently encounter in clinical practice.
AI-Enabled Collaboration and Global Knowledge Sharing in Dermatology
AI opens the doors for collaborative learning on a global scale by connecting students with peers and experts from around the world.6 This technology enables students to share cases, discuss diagnoses, and learn from a diverse community. With interactive case discussions, AI not only organizes and moderates these sessions but also ensures that they are focused and cover essential learning points, making the learning experience more engaging and productive.
AI-Enhanced Clinical Decision Support in Dermatology Training
AI can be a helpful guide in clinical decision-making, offering suggestions for possible diagnoses and treatment options based on the information provided. This feature not only supports students but also helps them learn and understand how medical decisions are made in practice. According to a study by Cheng CT, et al., AI-assisted images in medical education and diagnostics have shown to give more accurate clinical assessment results compared to traditional methods.7
Furthermore, AI can help students learn to integrate patient data from Electronic Health Records (EHR) into their diagnostic and treatment planning, making these processes smoother and more informed, while also using raw data from EHRs to develop prognostic models for better patient care.8
Optimizing Time Management and Efficiency with AI in Medical Training
AI significantly enhances time management and efficiency in medical education. By taking over automated administrative tasks like scheduling, documentation, and data entry, AI frees up students' time, allowing them to concentrate more on learning and patient care. Additionally, AI can streamline study plans by pinpointing high-yield topics and tailoring study schedules to align with exam dates and curriculum needs, ensuring a more focused and productive learning experience.
Final Thoughts on AI's Impact in Dermatology Education
In conclusion, the integration of AI in dermatology education offers a transformative approach, enhancing diagnostic accuracy, personalized learning, and clinical skills. AI's ability to provide real-time feedback, access to the latest research, and streamlined study plans empowers medical students to excel. As AI continues to evolve, its role in medical education will likely expand, providing even greater support and opportunities for future healthcare professionals.
Study Methodology
An online questionnaire (Google Survey) containing questions on 20 different dermatology cases was compiled with an overview image and a close-up image of skin lesions sent to the First Derm online platform, including a brief clinical description provided by the patients (Figure 1). The following areas of inquiry were used to collect data.
- Three differential diagnoses in the order of probability
- Recommendations on management
- Opinion on dermatologist/GP referral/ self treatment
- Time spent on each case
A second questionnaire was made using the same questions on the same cases, with the addition of 5 possible AI generated answers ranked in order using Autoderm version 2.2. (Figure 2).
Two groups of medical students were instructed to review the details provided, and answer the questions. Ten medical students received a questionnaire with 2 images and describing text of the patient's concern (Group A). A second group of 10 medical students received the same information and an AI assistance answer on the case (Group B). Each student was advised to fill out the online questionnaire based on their knowledge, while the Group B students had the opportunity to look at the AI generated answers and take the information into consideration when forming their own diagnoses.
At the end of the survey, information on the level of difficulty was obtained from both groups, while additional information on helpfulness of AI assistance in diagnosing the conditions, and opinion on using AI assistance were collected from the Group B students.
Correct diagnoses of the cases were obtained from board certified dermatologists via the First Derm online platform, to help determine the diagnostic accuracy of study and control groups. The data obtained from the two groups were assessed to determine the comparative accuracy of differential diagnoses, management recommendations and time spent on each case.


Results
1. Top Diagnosis Accuracy
The top diagnostic accuracy of 14 out of 20 cases were increased with AI assistance. 3 out of 20 cases had similar accuracy in both groups. The variation in accuracy in individual cases with and without AI assistance is shown in the graph below. (Figure 3)

2. Accuracy of top 3 differential diagnoses
The accuracy of top 3 differential diagnoses of 15 out of 20 cases were increased with AI assistance. The variation in accuracy of top 3 differential diagnoses in individual cases with and without AI assistance is shown in the graph below. (Figure 4)


Accuracy of management recommendations
Details on management recommendations including several classes of medication (eg: antibiotics, antifungals, moisturiser, corticosteroids) were obtained and compared to the dermatologists' recommendations. In 16 out of 20 cases, the recommendations were more accurate in the study group with AI assistance, while 2 out of 20 cases showed similar accuracy in both groups. (Figure 6)

Time taken for diagnosis and recommending management options
The average time spent on each case was significantly reduced in the study group with AI assistance, compared to the control group. (Figure 7)

Students' feedback
Majority of the participants in the study group who received AI assistance had positive feedback on performance and utility of AI. 4 out of 10 students claimed the use of AI alone would have been sufficient to resolve the consultation. 9 out of 10 students confirmed that they used the assistance given by the AI in completing the survey, and confirmed that the use of AI helped them to think about other differential diagnoses. 8 out of 10 students stated that they would use the AI in similar settings. The level overall of difficulty as recorded by the students was higher in the control group who did not receive any AI assistance. Overall, the study group with AI assistance completed the task with better accuracy and more efficient time management than the control group.




Discussion
This study assessed the impact of AI assistance on the diagnostic accuracy, management recommendations, and time efficiency of medical students in dermatology cases. Group A spent more time on the cases, got more diagnoses wrong, treatment wrong than Group B that had patient history and an AI assistant answer.
Key Findings
- Diagnostic Accuracy: AI assistance improved the top diagnostic accuracy in 14 out of 20 cases (75%) and improved the accuracy of the top three differential diagnoses in 15 out of 20 cases (75%).
- Management Recommendations: The AI-assisted group provided more accurate management recommendations in 16 out of 20 cases (75%), with similar accuracy in two cases.
- Time Efficiency: AI assistance significantly reduced the time spent on diagnosis and management compared to the control group (40%).
- Student Feedback: In general they thought the test was difficult, however Group B students thought it was less difficult when they had access to the AI assistant's answer. Most students found the AI to be useful when considering alternative diagnoses. Ninety percent of the medical students indicated they would use AI in a future diagnostic setting.
Conclusion
Overall, the AI-assisted group outperformed the control group in terms of diagnostic accuracy, efficiency, and decision-making confidence. This suggests that AI can be a valuable tool in enhancing medical education and clinical practice.
References
- Alex Krizhevsky, Ilya Sutskever, and Geoffrey E. Hinton. 2017. ImageNet classification with deep convolutional neural networks. Commun. ACM 60, 6 (June 2017), 84–90. https://doi.org/10.1145/3065386
- Bulathwela S, Pérez-Ortiz M, Holloway C, Cukurova M, Shawe-Taylor J. Artificial Intelligence Alone Will Not Democratise Education: On Educational Inequality, Techno-Solutionism and Inclusive Tools. Sustainability. 2024; 16(2):781. https://doi.org/10.3390/su16020781
- Sohail N, Puyana C, Zimmerman L, Tsoukas MM. AI in Dermatology: Bridging the Gap in Patient Care and Education. Clin Dermatol. Published online June 25, 2024. < href="https://doi:10.1016/j.clindermatol.2024.06.009" target="_blank">https://doi:10.1016/j.clindermatol.2024.06.009
- Wang T, Lund BD, Marengo A, Pagano A, Mannuru NR, Teel ZA, Pange J. Exploring the Potential Impact of Artificial Intelligence (AI) on International Students in Higher Education: Generative AI, Chatbots, Analytics, and International Student Success. Applied Sciences. 2023; 13(11):6716. https://doi.org/10.3390/app13116716
- Igbokwe, I.C., 2023. Application of artificial intelligence (AI) in educational management. International Journal of Scientific and Research Publications, 13(3), pp.300-307. https://www.ijsrp.org/research-paper-0323.php?rp=P13512782
- Sapci AH, Sapci HA. Artificial Intelligence Education and Tools for Medical and Health Informatics Students: Systematic Review. JMIR Med Educ. 2020;6(1):e19285. Published 2020 Jun 30. https://mededu.jmir.org/2020/1/e19285/
- Cheng CT, Chen CC, Fu CY, et al. Artificial intelligence-based education assists medical students' interpretation of hip fracture. Insights Imaging. 2020;11(1):119. Published 2020 Nov 23. https://insightsimaging.springeropen.com/articles/10.1186/s13244-020-00932-0
- Liopyris, Konstantinos, et al. "Artificial intelligence in dermatology: challenges and perspectives." Dermatology and Therapy 12.12 (2022): 2637-2651. >https://link.springer.com/article/10.1007/s13555-022-00833-8


